|
|
||||||||
| UDK 616.133-06 : 616.8 | ISSN 0350-2899, 29(2004) 1 p.5-7 | |||||||
Original paper Relationship between Severity of Neurological Status and Changes in Carotid Arteries in Coronary PatientsMilan Đorić, Branko Lović, Ivan Tasić, Danilo Stojiljković Summary: |
||||||||
| Napomena: sažetak na srpskom jeziku | ||||||||
IntroductionCerebrovascular accidents in all their clinical manifestations are on the third place among total mortality causes, just after cardiovascular diseases and malignant neoplasms. It's incidence is 160:100000 and its growing exponentially; males are on five time greater risk then females. Carotid arteries are responsible for a respectable percentage of cerebrovascular accidents; 9% is located in truncus brachiocephalicus, 12% in common carotid artery, 42% in bulbus and 37% in arteria carotis interna (1, 2). Last decade and more, carotid diseases is a field of great interest for a clinical doctors of different specialities (internists, neurologist, surgeons etc) as well as epidemiologist. Important fact is that risk factors for coronary, carotid and cerebrovascular disease are practically common. Knowing the fact that big percentage of asymptomatic forms is present and that very often those two entities are present in one patient, it's absolutely reasonable to search and estimate the presence and severity of them. AimThe aim of the study was to estimate the presence, severity and importance of neurological accidents in coronary patient due to carotid disease. Material and methodAmong 52 pts., all with angiographicly proved coronary disease, there were 38 males and 14 females, average age 57+-5 years. All of them were examined using method of colour Doppler echosonographie on Accuson-Sequoa C 256, using linear transducer 7,5 -10 MHz with 50 mm tissue penetration. Carotid arteries were in detail examined from their separation points up to their penetration in to the skull. Significance of the changes was expressed by stenosis grade, bilaterality of the changes and with characteristics and composition of the plaque. Also, all patients had survived some neurological accident, from transistor ischemic attack to major stroke with serious neurological deficit, what was verified by contrasted computerised tomography of the endocranium and with detail clinical neurological examination. Patients with conditions which also could be a cause for neurological accidents such as atrial fibrillation, valvular and haematological disease were excluded from the study. All invasive and computerised tomography examinations were done in Institute for CVD "Sremska Kamenica", "Dedinje" and Military Medecine Academy in Belgrade. Echosonography examinations had been done in Institute "Niska Banja" in Niska Banja. ResultsAmong 52 pts., 12 (23,07%) had TIA - group A, 34 (65,38%) had minor stroke
– group B and 6 (11,53%) had major stroke with severe neurological deficit
– group C. In a group A average stenosis was 34%, in B group it was 52%
and in a C group it was 78%. Bilateral changes were not present in a A
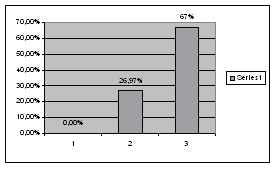
group, in a B group 9 (26,47%) and in a C group 4 (66,66%) were present.
Complicated plaque was present only in a C group — 1 (16,66%) patient. DiscussionMany authors proved direct connection between neurological status and
severity of carotid disease. Its well known and generally accepted that
major determinants for severity of plaques on carotid arteries are
percentage of stenosis, complicated and bilateral stenosis, specially when
more than one is present (3, 4, 5). Rupture of the plaque in 88% leads to
TIA or even more, in 92 % to complete cerebrovascular accident (6). In
our work there is a clear distribution of hemodinamicly significant
stenosis in group with major strokes, its positively correlating with
bilateral changes, too (figure 1).
|
||||||||
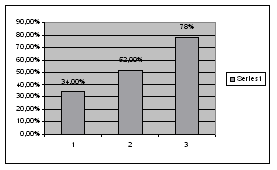 |
Figure 1. Distribution among study group
according to neurological status |
|||||||
 |
 |
|||||||
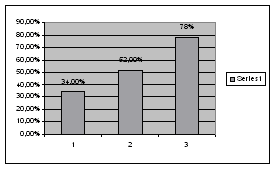
| Grafik 2 Average stenosis distribution among study groups | Grafik 3. Percentage distribution of bilateral changes in study groups | |||||||
|
Very significant is that the only patient with complicated plaque was also in a major stroke group and that there was not such a patient in a groups B and A (grafik 2). Those facts are comparatable with other authors and literature (7, 8). Anyway, one fact is important to be underlined: its practically vitium artis to underestimate lessions under 50%, because, very often, such a plaques are not significant in haemodinamic aspect, but, they are soft, lipid-full, fragile and with a thin cover and they can easily get ruptured. However, in a such patients, on CT examinations we can find few small, lacunar, subcortical, diffuse ischemic leasions in brain tissue, which can be presented by atypical and abortive clinical presentation (confusion, headache, vertigo etc), or even, some rupture of the plaque if so called "silent brain zones“ are affected can go asymptomatically (8, 9). All this facts bring us to knowledge that, in patients with risk factors, coronary as well as neurological patients detail clinical and ultrasound examination of carotid arteries should be done. Those facts are solid basis for optimal and rational treatment strategy, no matter conservative or surgical. Statins, antiplatelets and ACE inhibitors are "golden trio“ for modern medicament treatment. Surgical endartherectomy is reserved for symptomatic patients with stenosis over 70% or asymptomatic with stenosis over 80% and multiple risk factors (10). Stenting is reserved for elderly or patients on a higher operative risk. Conclusion
References
Corresponding Address: |
||||||||
|
|
||||||||
| Infotrend Crea(c)tive Design | Revised: 20 May 2009 | |||||||
